Air pollution confounding factors
The Kincade Fire in northern Sonoma County started on October 23, 2019, was contained on Nov. 6 but continued to burn and affect the test location during and after the SSHS study was finished.
Because PM 2.5 is a potent inflammatory agent, a monitoring device was purchased to track indoor air quality and activated the day before the first (baseline) blood draw.
This ad-free article is made possible by the financial support of the
Center for Research on Environmental Chemicals in Humans: a 501(c)(3) non-profit.
Please consider making a tax-deductible donation for continued biomedical research.
PM2.5 is used to make health recommendations
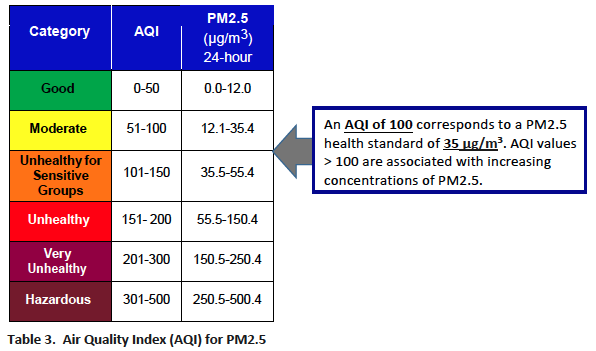
AIR QUALITY INDEX (AQI)The following text and Figure 3, from the California Department of Public Health (PDF)
“The US EPA created the Air Quality Index (AQI) to communicate information about air quality to the public.10 The AQI communicates the health impacts of air pollutant concentration using a 6-level color system (Green, Yellow, Orange, Red, Purple and Maroon).
“Each color-coded level has an associated descriptive term, progressing from “Good” to “Hazardous.” For each pollutant, the AQI scale value of 100 corresponds to the 24-hour primary health standard. The AQI is most often displayed for two pollutants, PM2.5 and ozone. For PM2.5, the 24-hour health standard of 35 μg/m3 corresponds to the AQI value of 100; AQI values greater than 100 indicate increasing levels of health risk, beginning with “Sensitive
Groups” in the Orange category and progressing to “Everyone” in the Red, Purple, and Maroon categories. See Table 3 below.”
In retrospect, activities probably should have been restricted before the baseline draw.
However, a literature search has not found a reference dealing with the pharmacokinetics of PM 2.5. It is, at this point, unknown how long a pre-baseline isolation period would need to be for an un-confounded valid baseline.
Accordingly, outdoor activity was limited during the trial because of wildfire smoke pollution.
In addition, a new HVAC filter was installed and two stand-alone HEPA air purifiers employed at the trial location to keep indoor air in the range of healthy as defined by
Because outdoor activities were not restricted before the trial, the baseline hsCRP was probably affected, contributing to an unhealthy baseline measurement.
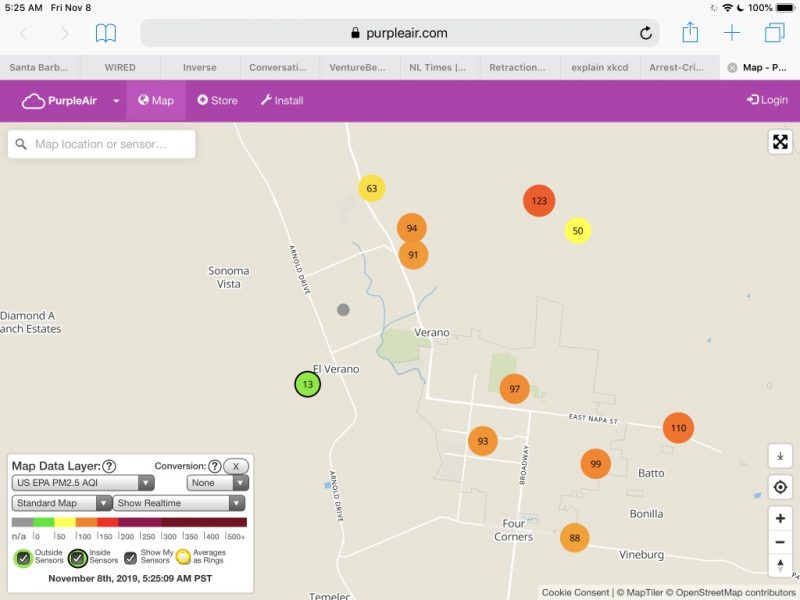
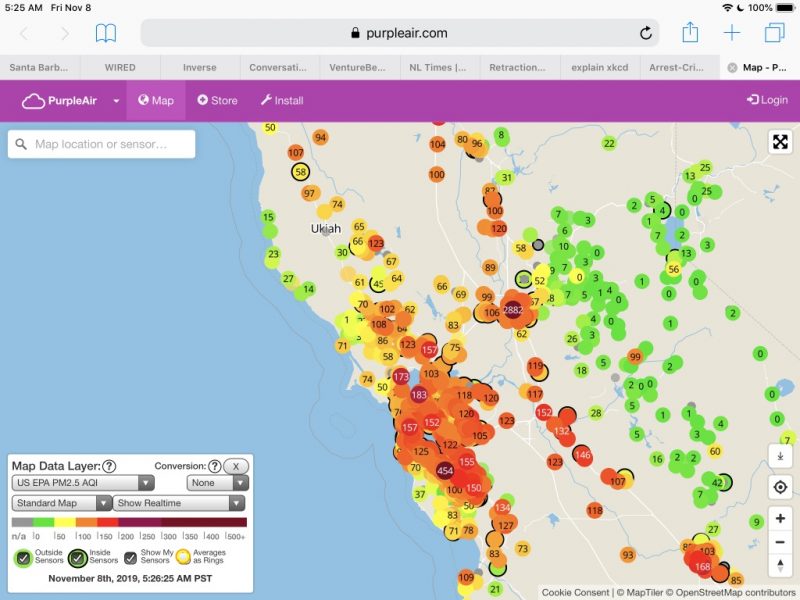
In addition, the air was extremely unhealthy on the North coast on Nov. 8: the date of the first blood draw and the first day of the “Typical” diet. Significant to the PM 2.5 exposure is that the blood sample for BPA and other toxics testing needed to be delivered to the lab at UCSF Mt. Zion within four hours of the draw.
Because the test subject and investigator were the same person, that means that the scientist/lab rat had to be exposed to extremely unhealthy PM 2.5 for at least 3 hours including the commute into San Francisco and the deliveries of blood samples to the lab and the hsCRP sample to the lab at the Parnassus campus.
More air quality snapshots are available at: Air quality exposure may have confounded results.
Restriction of outdoor exercise meant forgoing regular exercise such as jogging. The lack of that exercise and the effect of being “trapped” had a noticeable effect on SSHS subject psychological stress.
- Home, & Office — cooking, vinyl flooring, wall coverings, upholstery, and other plastic-based products, pet dander, printer toner.
- External – Smog, wildfires.